
04 May Seamless Patient Referrals and Transitions of Care
Providing quality pediatric care takes collaboration between parents and primary care physicians (PCPs), and effective management of referrals and transitions of care is vital to the success of that partnership. Having a complete health record for every patient is a primary principle of the Patient-Centered Medical Home concept. Without it, it’s impossible for PCPs to deliver the best care to children.
The Law of Cause and Effect
The point is not that patients and their parents seek outside care, whether with or without referrals, but that the results of that care be incorporated into the record. Patients get care outside the practice for a number of reasons, including:
- When a need arises for specialist tests, diagnosis, or therapy beyond the scope of the PCP
- As a result of visiting an urgent care center or ER
- Because of hospital inpatient treatment
Whether outside care is initiated by the patient and the PCP didn’t know about it, or it was initiated through a referral and the PCP did know, the onus remains with the PCP to follow up and maintain a complete patient health picture.
To do this, the PCP needs to ask questions, create and send the referral, track the progress of referrals, and follow up on reports from other providers. There are multiple risks associated with not doing so, not least the potential loss of patient life.
Mapping the Referral Lifecycle
Most PCP referrals follow a fairly standard cycle, which begins with the generation of the referral and sending it to the outside care provider.
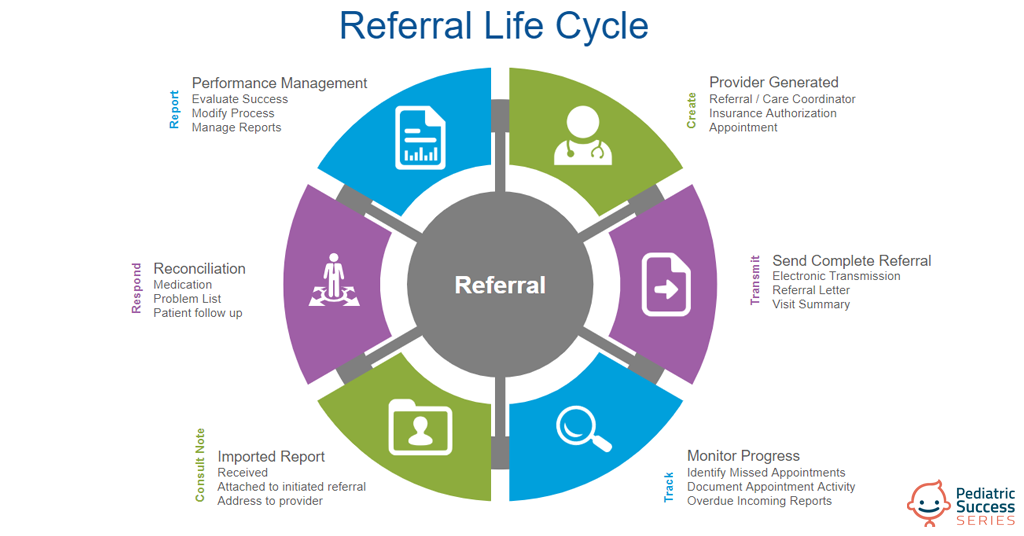
Tracking should begin almost immediately to determine whether appointments are made and kept, and reports sent to all parties. After receiving a report, it needs to be imported into the patient’s health record and, at this point, any new medications, problems, and planned follow-ups need to be reviewed by a clinician. When everyone involved takes ownership and meets these “business rules,” it minimizes the chance for patients to fall through the cracks.
Preventing Adverse Results
Here’s an example of the kind of adverse results that could happen if referrals aren’t managed effectively.
During a visit, the PCP hears a suggestion of an irregular heartbeat in a teen who is an athlete and who appears to be healthy. She refers the patient to a cardiologist to investigate because of reported family heart conditions. Whether the patient goes or not, the practice receives no report and therefore does no follow-up. The patient plays basketball, has a heart attack and dies on the court. If the PCP had followed up and made sure he was evaluated, and had taken the necessary steps to either confirm or deny their concern, they could possibly have prevented this sudden cardiac death if they were more persistent in making sure he got the appropriate consultation with cardiology.
That’s not the only risk, either. Malpractice suits are common, and they can be precipitated by much smaller oversights than this. When PCPs refer patients to an outside provider it’s because they have good reason to do so. From the moment a PCP says “you need to see a specialist,” even if there’s no record of that comment in the EHR, it becomes their responsibility to follow up. That’s not a reason to avoid documenting the concern, however; in fact, having pediatric-specific documentation can often provide you with a safety net during an allegation of malpractice.
Self-Referral Patients
And what about patients who refer themselves to outside care providers? Just because the PCP wasn’t aware of the referral doesn’t mean they can ignore it. Every PCP should get comfortable with asking the question “Have you had any other medical care since I last saw you?” You should educate your patients to not only expect it, but to answer it fully.
Close the Referral Gap
Following up on patient referrals is another way to ensure patients are getting the care they need. This may also be an opportunity to fill your practice’s schedule with patient visits.


